Refining T cell biology to develop powerful biologics


Scroll Down
T Cell Biology
T cells are a type of white blood cell that are an essential part of your immune system and play a central role in the adaptive immune response.



One type of T cell acts as ‘killer cells’, attacking cells infected by a virus or other pathogen which they recognise through fragments of foreign proteins (antigens) displayed on the surface of these cells.
Once the threat has gone, these T cells become dormant. Some will remain as memory cells for many years: if the threat returns, your immune system can recognise it and fight it off quickly.



Scroll Down


T cells play an important role in fighting cancer.
A normal cell transforms into a cancer cell through a series of mutations in its DNA. These result in changes to the protein fragments displayed on the surface of the cancer cell.
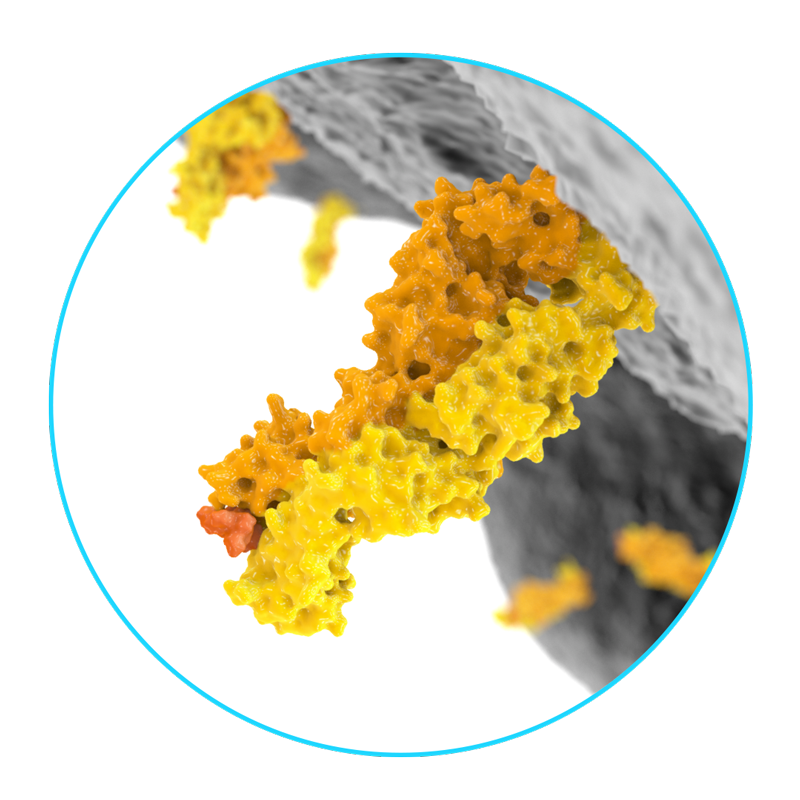
Mutated protein fragments, known as neoantigens, can be recognised by T cells but most of the fragments – although cancer specific – are not recognised.
These fragments are derived from genes which are re-expressed in the cancer cell and recognised as “self”. Owing to this process, tumours are able to evade the immune system to grow and spread.




Scroll Down

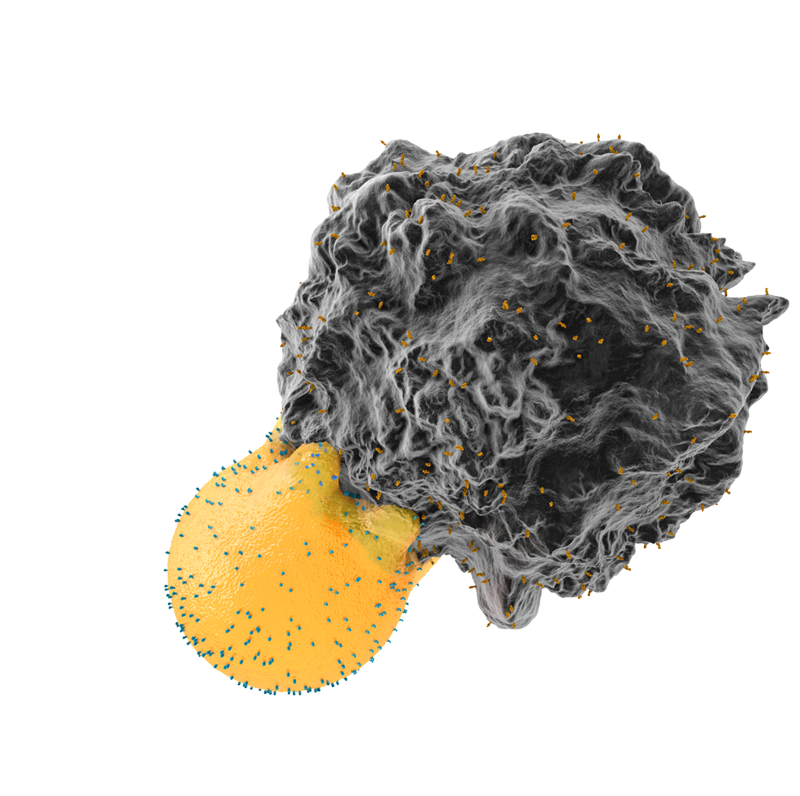

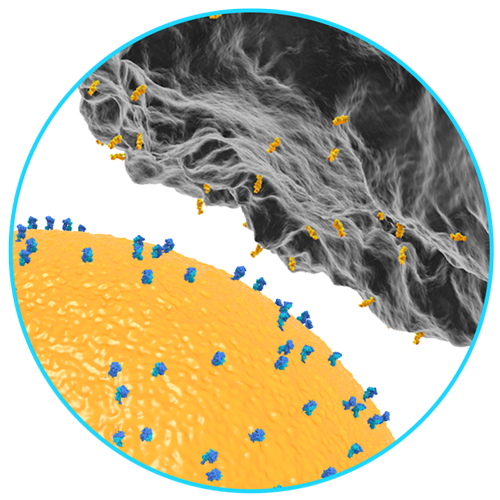
The part of the T cell that binds to a foreign antigen or cancer neoantigen is called the T cell receptor (TCR). It is this binding of the TCR to an antigen that causes T cell activation, proliferation and differentiation.
Advances in our understanding of T cell biology have enabled the development of immuno-oncology drugs such as check point inhibitors. These work by stimulating the response to cancer neo-antigens but they are unable to overcome the inability to recognise the cancer-specific “self” antigens.
The approach we are using to target cancer cells is also being developed for autoimmune conditions – although in this case we are aiming to suppress inflammation in a highly specific manner.
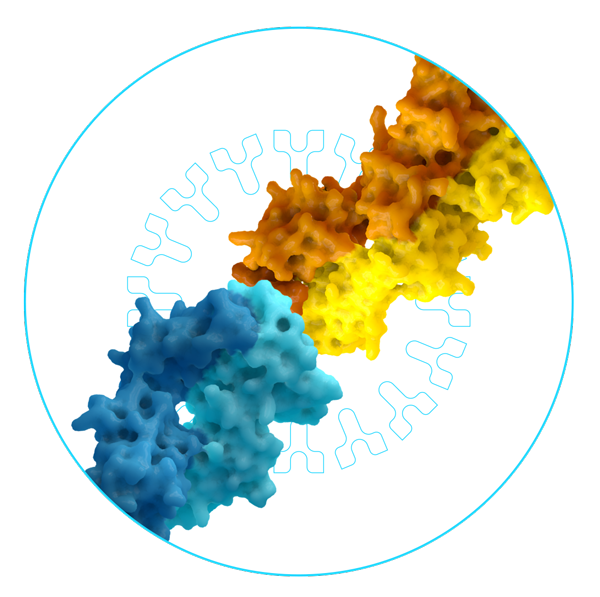
T-Therapeutics is developing drugs which can recognise these self-antigens and re-direct T cells to kill these cancer cells.




Scroll Down

Our Platform
Best-in-class transgenic mouse platform combined with disease-to-target discovery approach.

Our goal is to treat cancers that are currently untreatable – reshaping the clinical landscape for cancer patients.


